FEMALE LAPAROSCOPY
INTRODUCTION
An examination of a woman’s internal pelvic structure can provide important information regarding infertility and common gynecologic disorders. Problems that cannot be discovered by an external physical examination may be discovered by laparoscopy and hysteroscopy, two procedures that provide a direct look at the pelvic organs. These procedures may be recommended as part of your infertility care, depending on your particular situation. Laparoscopy and hysteroscopy can be used for both diagnostic (looking only) and operative (looking and treating) purposes.
Diagnostic laparoscopy may be recommended to look at the outside of the uterus, fallopian tubes, ovaries, and internal pelvic area. Diagnostic hysteroscopy is used to look inside the uterine cavity. If an abnormal condition is detected during the diagnostic procedure, operative laparoscopy or operative hysteroscopy can often be performed to correct it at the same time, avoiding the need for a second surgery. Both diagnostic and operative procedures should be performed by physicians with surgical expertise in these areas. The following information will help patients know what to expect before undergoing any of these procedures.
DIAGNOSTIC LAPAROSCOPY
Laparoscopy can help physicians diagnose many gynecological problems including endometriosis, uterine fibroids and other structural abnormalities, ovarian cysts, adhesions (scar tissue), and ectopic pregnancy. If you have pain, history of past pelvic infection, or symptoms suggestive of pelvic disease, your physician may recommend this procedure as part of your evaluation. Laparoscopy is sometimes recommended after completing an initial infertility evaluation on both partners. It is usually performed soon after menstruation ends.
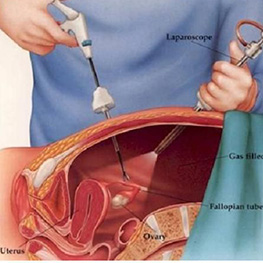
Laparoscopy is usually performed as daycare basis under general anesthesia. After the patient is under anesthesia, a telescope is placed through the navel. Carbon dioxide gas is used to fill the abdomen, which pushes the abdominal wall away from the internal organs and decreases the risk of injury to surrounding organs such as the bowel, bladder, and blood vessels. Occasionally, alternate sites may be used for the insertion of the laparoscope based upon physician experience or the patient’s prior surgical or medical history. These incisions are typically small (usually less than 1 inch in length). While looking through the laparoscope, the physician can see the reproductive organs including the uterus, fallopian tubes, and ovaries.
A small probe is usually inserted through another incision, in the lower abdomen, in order to move the pelvic organs into clear view (Figure 2). Additionally, a fluid is often injected through the cervix, uterus, and fallopian tubes to determine if the tubes are open. If no abnormalities are noted at this time, one or two stitches close the incisions. If abnormalities are discovered, diagnostic laparoscopy can become operative laparoscopy.
OPERATIVE LAPAROSCOPY
During operative laparoscopy, many abdominal disorders can be treated safely through the laparoscope at the same time that the diagnosis is made. When performing operative laparoscopy, the physician inserts additional instruments such as probes, scissors, grasping instruments, biopsy forceps, electrosurgical or laser instruments, and suture materials through two or more additional incisions. Lasers, while a significant help in certain operations, are expensive and are not necessarily better or more effective than other surgical techniques or tools used during operative laparoscopy. The choice of technique and instruments depends on many factors, including the physician’s experience and preference and location of the problem. Some problems that can be attempted to be corrected with operative laparoscopy include treating adhesions (scar tissue) from around the fallopian tubes and ovaries, opening blocked tubes, removing ovarian cysts, and treating ectopic pregnancies. Endometriosis can also be removed or destroyed from the outside of the uterus, ovaries, or peritoneum. Under certain circumstances, fibroids on the uterus may also be removed. Operative laparoscopy can also be used to remove diseased ovaries and damaged fallopian tubes.
An increasing number of surgeons are performing hysterectomies with robotic assistance (robotic-assisted laparoscopy). However, robotic surgery is more expensive and generally more time-consuming than conventional surgery, and not all hospitals have this equipment available. It is also possible that evolving health-care changes will affect the availability of robotic and other “high-tech” procedures. Operative instrument Laparoscope Uterus.
Risks of Laparoscopy
Similar to all surgeries, there are risks associated with laparoscopy. Postoperative bladder infection and skin irritation are most common. Adhesions (scar tissue within the abdomen) may develop, although this is less likely than after an open procedure (laparotomy). Hematomas (bloodfilled bruising) of the abdominal wall can occur near the incisions. Pelvic or abdominal infections may occur. Serious complications of diagnostic and operative laparoscopy are rare. The major risk is damage to the bowel, bladder, ureters, uterus, major blood vessels, or other organs, which may require additional surgery. Injuries can occur during the insertion of various instruments through the abdominal wall or during the operative treatment. Certain conditions may increase the risk of serious complications. These include previous abdominal surgery, especially bowel surgery, and a history or presence of bowel/pelvic adhesions, severe endometriosis, pelvic infections, obesity, or excessive thinness. Allergic reactions, nerve damage, and anesthesia complications rarely occur. Postoperative urinary retention is uncommon and venous thrombosis (blood clot) is rare. The risk of death as a result of laparoscopy is very small (around 3 in 100,000). When all possible complications are considered, 1 or 2 women out of every 100 may develop a complication, usually of minor consequence.
Postoperative Care
Following laparoscopy, the navel area (belly button) is usually tender and the abdomen may be bruised and tender. Gas used to distend the abdomen may cause discomfort in the shoulders, chest, and abdomen. Anesthesia can cause nausea and dizziness. The amount of discomfort depends on the type and extent of procedures performed. Normal activities can usually be resumed within a few days. Significant abdominal pain, worsening nausea and vomiting, a temperature of 101°F or higher, drainage of pus from an incision, or significant bleeding from an incision are potential serious complications requiring immediate medical attention.
CONSIDERING OPERATIVE LAPAROSCOPY VERSUS LAPAROTOMY FOR PELVIC SURGERY
Many gynecologic operations are performed via laparotomy, in which an incision (“bikini” or “up and down”) is made to open the abdomen. Patients generally remain in the hospital for a few days following surgery and may return to work in 2 to 6 weeks, depending on the level of physical activity required. Many gynecologic procedures can also be performed by operative laparoscopy. Following operative laparoscopy, patients are generally able to return home the day of surgery and recover more quickly, returning to full activities in 3 to 7 days.
Some types of operations may be too risky to perform laparoscopically, while in others it is not clear that laparoscopy yields results as good as those by laparotomy. The surgeon’s experience and available resources also play a role in deciding whether operative laparoscopy or laparotomy should be used. When considering a gynecologic operation, the patient and her doctor should discuss the pros and cons of performing a laparotomy versus an operative laparoscopy.
DIAGNOSTIC HYSTEROSCOPY
Hysteroscopy is a useful procedure to evaluate women with infertility, recurrent miscarriage, or abnormal uterine bleeding. Diagnostic hysteroscopy is used to examine the uterine cavity (Figure 3), and is helpful in diagnosing abnormal uterine conditions such as fibroids protruding into the uterine cavity, scarring, polyps, and congenital malformations. A hysterosalpingogram (an x-ray using dye to outline the uterus and fallopian tubes), pelvic ultrasound or sonohysterogram (ultrasound with introduction of saline into the uterine cavity), or an endometrial biopsy may be performed to evaluate the uterus prior to hysteroscopy.
The first step of diagnostic hysteroscopy often involves slightly stretching the canal of the cervix with a series of dilators to temporarily increase the size of the opening. The hysteroscope (a long, thin, lighted, telescopelike instrument) is inserted through the cervix and into the uterus. Skin incisions are not required for hysteroscopy. Carbon dioxide gas or a fluid such as saline are then injected into the uterus through the hysteroscope. This gas or fluid expands the uterine cavity and enables the physician to directly view the internal structure of the uterus. Diagnostic hysteroscopy is an outpatient procedure that is performed in a physician’s office or operating room. It is often performed soon after menstruation has ended because the uterine cavity is more easily evaluated.
OPERATIVE HYSTEROSCOPY
Operative hysteroscopy can treat many of the abnormalities found during diagnostic hysteroscopy or on other imaging studies. Operative hysteroscopy is similar to diagnostic hysteroscopy except that narrow instruments are placed into the uterine cavity through a channel in the operative hysteroscope. Fibroids, scar tissue, and polyps can be removed from inside the uterus. Some structural abnormalities, such as a uterine septum, may be corrected through the hysteroscope.
Your physician may want you to take medications to prepare the uterus for surgery. At the conclusion of surgery, your physician may insert a balloon catheter or other device inside the uterus. Antibiotics and/or estrogen may be prescribed after some types of uterine surgery to prevent infection and stimulate healing of the endometrium. Endometrial ablation, a procedure in which the lining of the uterus is destroyed, can be used to treat some cases of excessive uterine bleeding. Ablation of the uterine lining is not performed in women who wish to become pregnant.
Risks of Hysteroscopy
Complications of hysteroscopy occur in about 2 out of every 100 procedures. Although still uncommon, perforation of the uterus (a small hole in the uterus) is the most common complication. Although perforations usually close spontaneously, they may cause bleeding or rarely result in damage to nearby organs, which may require further surgery. Uterine cavity adhesions or infections may develop after hysteroscopy. Serious complications related to the fluids used to distend the uterus include fluid in the lungs, blood clotting, fluid overload, electrolyte imbalance, and severe allergic reactions. Severe or life-threatening complications, however, are very uncommon. Some of the complications above may prevent completion of the surgery.
Postoperative Care
Following hysteroscopy, some vaginal discharge or bleeding and cramping may be experienced for several days. Most physical activities can usually be resumed within 1 or 2 days. You should ask your physician when to resume sexual intercourse. If a balloon catheter is left in the cavity, it is usually removed after several days. As noted above, antibiotics and/or estrogen may be prescribed after surgery.
CONCLUSION
Laparoscopy and hysteroscopy allow physicians to diagnose and correct many gynecologic disorders on an outpatient basis. Patient recovery time is brief and significantly less than the recovery time from abdominal surgery through larger incisions. Before undergoing laparoscopy or hysteroscopy, patients should discuss with their physicians any concerns about the procedures and their risks.
Service Brief
With the advent of cutting-edge technology, it has become a feasible option to perform ‘minimally invasive’ surgeries with precision and finesse. Laparoscopy and Hysteroscopy are two such surgeries used to diagnose and cure certain female infertility conditions.
Laparoscopy: It is done using a small but significant telescope named ‘Laparoscope’ to which a light source and camera are attached. It enables doctors to see ovaries, outside of uterus and fallopian tubes inside the abdomen. The doctors can perform surgeries while looking inside the abdomen. Laparoscopy is done to determine the causes of infertility. The doctors use this technique to treat cysts, endometriosis, blockage in the fallopian tubes and fibroids.
Hysteroscopy: A tool called ‘Hysteroscope’ is used to see inside the womb. Hysteroscopy is usually done to determine the cause of abnormal bleeding, causes of infertility, to remove growths in the uterus like fibroids & polyps, to resect septums. During the test, the doctor can find and treat the problem at the same time.
Service Information
We provide following fertility enhancing Endoscopic Procedures:
Diagnostic Hysteroscopy
Diagnostic Hysteroscopy + Laproscopy + Chromopertubation
Operative Hysteroscopy:
Hysteroscopic Polypectomy
Hysteroscopic Septum Resection
Hysteroscopic metroplasty
Hysteroscopic Adhesiolysis
Hysteroscopic Myomectomy
Operative Laproscopy:
Simple cysts Excision
Hydrosalpinx clipping/Excision
Cauterization of Endometriotic Spots
Fimbrioplasty / Tubal Adhesiolysis
Complex cysts (Choc / Dermoid)
Laparoscopic Myomectomy
Tubal Reanastomosis
Laparoscopic salpingectomy (ectopic pregnancy)